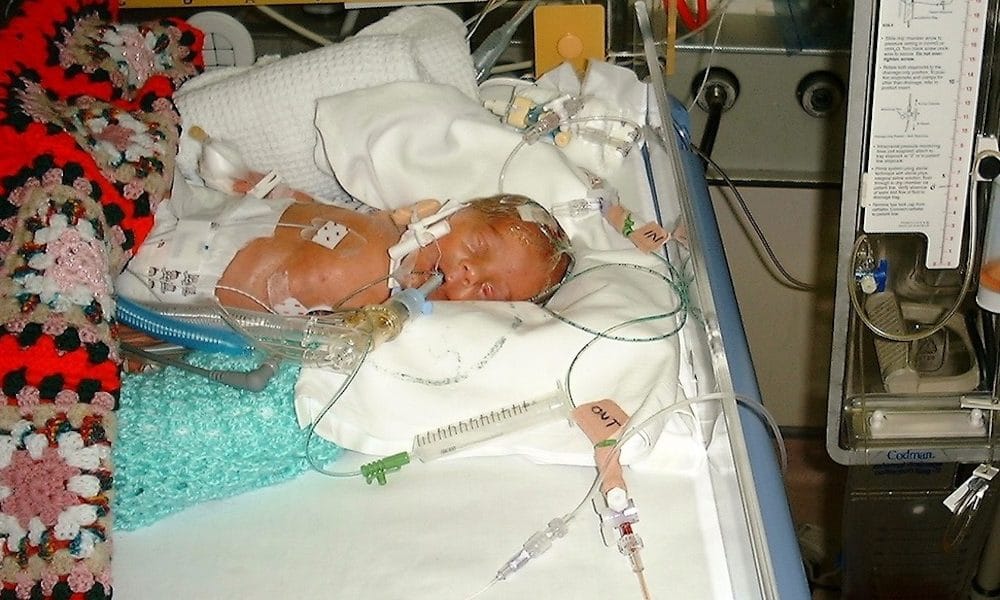
“But when he was 48 hours old, he had a massive brain haemorrhage on the right side of his brain and a small one on the left, and another in his lungs,” says Steve.
“We weren’t allowed to see him for that 48 hours – we were given a polaroid picture, but he was all battered and bruised and had wires coming out of him.”
Doctors told Becky and Steve that Isaac would need intervention, and suggested a new treatment they were trailing. Drift therapy was developed in 1998 and trialled from 2003 by Andrew Whitelaw, professor of neonatal medicine at the University of Bristol and Ian People, consultant neurosurgeon from University Hospitals Bristol and Weston NHS Foundation Trust.
Short for ‘Drainage, Irrigation and Fibrinolytic Therapy’, Drift treats babies with serious brain haemorrhage, known as intraventricular haemorrhage, which can lead to severe learning impairment and cerebral palsy. It aims to reduce disability by washing out the ventricles in the brain to remove toxic fluid and reduce pressure.
Bleeding into the fluid spaces of the brain is one of the most common consequences of being born prematurely. These bleeds are often further complicated, causing a high risk of learning difficulties and cerebral palsy.
“The doctors sat us down and explained what our options were, and we decided to give Isaac the best chance possible,” Steve says.
Steve and Becky, who live in Yate, Gloucestershire, signed a consent form to allow doctors to perform Drift, and then waited a couple of weeks until Isaac was strong enough for them to carry out the procedure.
“Things were a bit dicey and there was a point we didn’t think he’d make it,” Steve says.
“One evening, doctors told us they’d done everything they could and to expect a phone call. We went home from the hospital and didn’t sleep that night. In the morning, they rang and said he’d made an amazing recovery.”
Steve and Becky knew they were taking a risk, and doctors told them to prepare for the worst.
“We wanted to give him every opportunity,” Steve says. “We were hopeful it would help, but we knew we wouldn’t be able to see until he grew older.”
The procedure lasted around 28 hours, during which time Isaac was put under anaesthetic and hooked up to a clot-busting fluid that entered his brain. Steve and Becky were allowed to sit near him, and Steve remembers nurses coming in to make sure Isaac was okay.
After two months of slow recovery, Isaac was allowed home. At first, it was scary. Steve and Becky slept with the lights on, because that’s what Isaac was used to in hospital. Slowly, they all adjusted to their new lives. But as Isaac grew, they didn’t know what to expect.
“We weren’t completely aware of how the procedure could affect him, because the brain is so complex. We were looking for signs for everything – we were amazed at every milestone he got to, and each one meant more to us because we weren’t expecting him to do it,” Steve says. “And he’s carried that on throughout his whole life.”

Isaac Walker aged 19
Isaac has gone on to become one of dozens of babies who have helped to prove the treatment is worth the NHS investing in; this week, researchers published a ten-year follow-up in the journal Archives of Diseases in Childhood.
Researchers from Bristol Medical School assessed survivors from the group of premature babies with severe brain haemorrhage who were recruited for a trial that compared to babies given standard treatment using lumbar punctures to control expansion of the ventricles in the brain and reduce pressure.
Survival without severe cognitive disability was 66 percent in the Drift group and 35 per cent in the standard treatment group. They also found that infants given the DRIFT treatment were also more likely to attend mainstream education.
Steve isn’t surprised at the results, because he has ‘living proof’ that it works. Isaac, who has mild cerebral palsy on his left side, is now at university, studying software engineering, although
Steve isn’t completely surprised at Isaac’s latest milestone.
“We started to realise how special he was because of how doctors were reacting to his progress,” Steve says.
“Professor Whitelaw followed Isaac for many years, and has kept in touch. He’s used Isaac as an example when he’s given speeches about Drift, and shown his brain scans. He’s always been amazed by Isaac; he’s a man of few words, so we knew Isaac must have done really well because he was showing emotion.”
No one knows exactly what would have happened to Isaac if he hadn’t received the Drift treatment, but Steve knows their situation would be different.
“His brain wouldn’t have recovered and rewired the way it has,” he says.
While Steve doesn’t know why Isaac did particularly well on the treatment, he knows his determination has probably helped.
“He’s always been confident, and as a child he was very determined, which has helped him as he grew up. He’s taken everything in his stride, not worried about who he is and what he can and can’t do, and that’s probably helped him.”
Isaac describes the experience of being somewhat of a poster boy for the procedure as ‘weird’.
“It’s surreal to look back on something and think that if it didn’t happen, I wouldn’t be here,” he says.
“If I hadn’t got the Drift procedure, it would’ve made a massive difference in the way I live, but because I did, I don’t know any different to how I’ve grown up.”
He says his progress is a testament to the procedure, which has always been in the background. But there’s still a way to go before the NHS rolls out the treatment so it’s accessible for all premature babies who need it.
This will be a major effort, according to Dr Karen Luyt is leading the research team who carried out the 10-year follow up, after Whitelaw handed the responsibility to her when he retired.
It’s a complex treatment that can be damaging if it’s not carried out properly, and there will only be four centres in the UK where the Drain procedure can potentially be delivered. Luyt needs to now convince the National Institute of Clinical Excellence that they should fund the procedure for the NHS.








