Interdisciplinary goal setting in community neurorehabilitation: The importance of alignment

By Dr Liz Acland, neuropsychologist, Cognivate
Community neurorehabilitation requires complex therapy provision.
Case managers must frequently coordinate comprehensive programmes involving a range of specialist therapies, such as neuropsychology, occupational therapy, physiotherapy and speech and language therapy.
Each clinician brings specialist knowledge, discipline-specific formulations, and professional measures of progress.
However, when rehabilitation plans are developed in parallel between the disciplines, rather than in partnership with the client at the centre, rehabilitation can unintentionally become fragmented, and progress can falter.
At Cognivate, we believe the difference between multidisciplinary input and true interdisciplinary practice is subtle but clinically significant.
Our holistic, client-centred model is built on the principle that a team must work together to help clients achieve goals that are truly important to them.
When Good Therapy Becomes Disconnected
Following an acquired brain injury (ABI), a client’s rehabilitation needs will rarely sit neatly within one professional domain.
The person’s function will be affected by the interplay among their physical, cognitive, and communication impairments, which must then be considered within the individual’s wider social context and lifestyle.
If each therapeutic discipline sets goals independently, even if they are clinically sound, the overall programme can become fragmented.
It can lead to superfluous goals, excessive therapy load, conflicting advice, and unrealistic demands on the client’s time.
This can feel disjointed to the client, the family, the case manager and the therapists themselves, and ultimately result in slower progress towards meaningful outcomes.
Moving From Discipline-Specific Goals to Shared Objectives
True interdisciplinary goal-setting begins with a shared functional objective rather than professional priorities.
Teams should align around participation-based outcomes identified by the client, such as returning to an enjoyable leisure activity, a valued domestic task, re-establishing an important role or returning to work.
This allows each therapist to contribute their expertise to a single focus that is meaningful and valuable to the client. Each discipline retains its specialist expertise, but the direction is shared.
This cohesive approach can ensure rehabilitation is optimised.
A Case Study: Ben
The figure below illustrates the difference between a multidisciplinary and an interdisciplinary approach.
Ben was referred to Cognivate following a traumatic brain injury (TBI), which had left him with a range of physical, cognitive and communication impairments. To achieve his goal of increased activity levels, he required a comprehensive team of therapists.
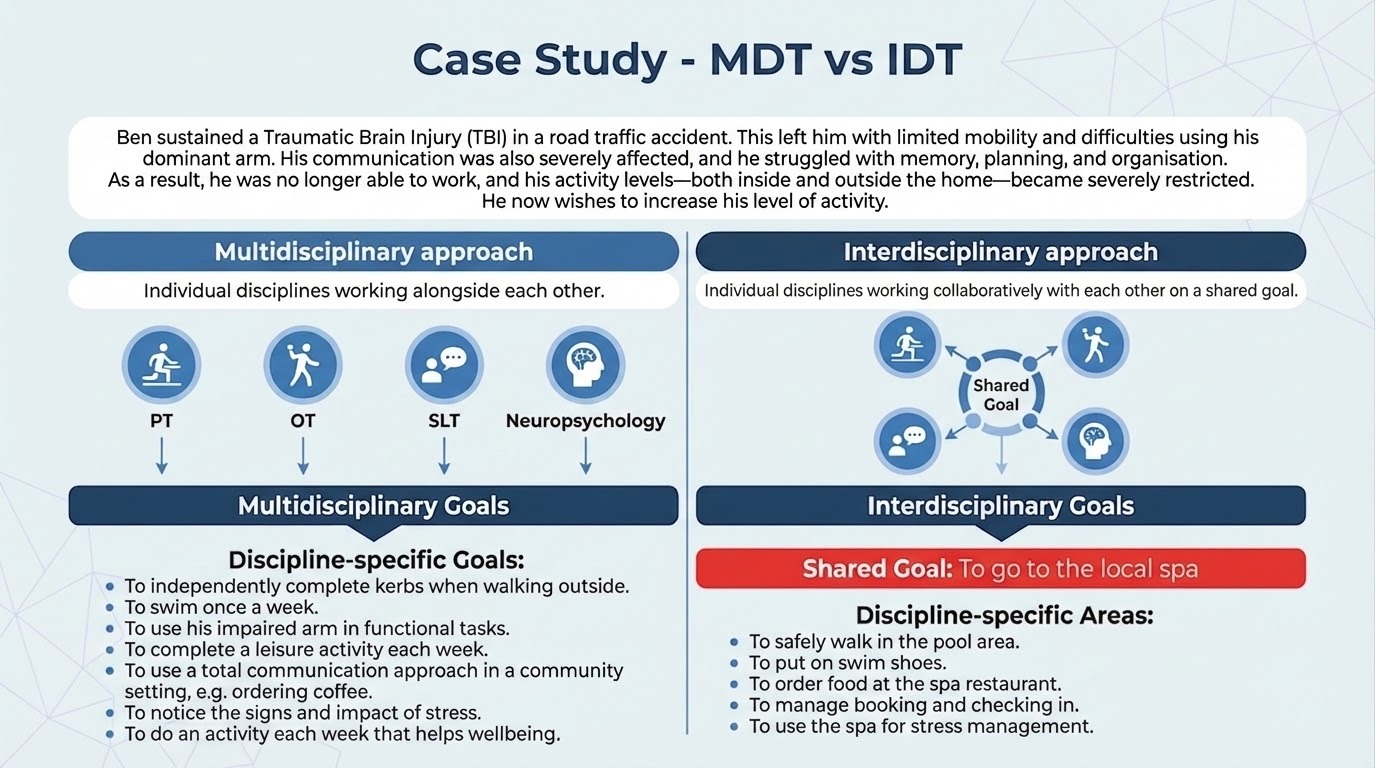
Traditional multidisciplinary models involve multiple disciplines setting separate short-term goals.
For Ben, this fragmented approach risked ‘goal overload,’ where a long list of unconnected tasks could have hindered, rather than helped, his rehabilitation.
Instead, the interdisciplinary team helped Ben identify a single, meaningful target: attending his local health spa. Each discipline then integrated their expertise to support this central goal:
- Physiotherapy: Focused on balance and gait to improve safety in the wet pool area and build strength for swimming.
- Occupational therapy: Completed a risk assessment of the spa environment, exploring compensatory strategies and safety measures with Ben and the team. ● Speech and language therapy: Assisted Ben in applying a “total communication” approach within the spa environment, targeting key interactions such as ordering food or asking for help.
- Neuropsychology: Supported Ben in using the spa as an active tool for managing stress.
While working towards this specific goal, Ben built a range of transferable skills that he was then able to apply to other rehabilitation targets.
The Cognivate Approach: Deliberate Coordination
Interdisciplinary goal setting does not happen organically; it requires deliberate coordination. Our model addresses this through several key structural elements:
- The Key Worker: Every client is assigned a key worker, typically from our core team. This individual maintains oversight of shared goals, coordinates the therapy team, and serves as a central point of contact for the client, family, and referrer.
- Integrated Assessment: Our process begins with an interdisciplinary assessment. After individual visits, the team meets for a “formulation session” to share findings and collaboratively identify the client’s key priorities.
- Goal-Setting Meetings: Within the first four weeks of treatment, the key worker arranges a joint session with the client and the full therapy team to finalise and agree on specific shared goals.
- Continuous Team Communication: We utilise integrated systems and shared electronic records to ensure information is “joined up” daily, allowing therapists to integrate each other’s work into their own sessions.
Beyond Therapy Hours
In complex brain injury rehabilitation, success is not defined by the number of sessions delivered. It is defined by whether those sessions collectively move a person closer to meaningful participation in the activity of their choice. An effective interdisciplinary team is an integral part of this process.
At Cognivate, our goal is to ensure therapy is not simply comprehensive but cohesive. By aligning our expertise around what genuinely matters to the individual, we provide a structured framework for progress that helps our clients return to as normal a life as possible.
Find out more about Cognivate at cognivaterehab.com









