
From her father’s battle with MND and a lack of appropriate care and support came Abbie Coutts’ desire to make a change within the medical profession. Here, she shares her story of becoming an educator, dedicated to equipping healthcare workers with greater ability to support patients and their families
“From a young age I was always determined not to be a nurse. My sister was a nurse, my mum worked in a care home and I decided that I was going to do something completely different.
“I left my childhood home of Cornwall to study Film at Kent University, Canterbury which I absolutely loved. When it became apparent that there weren’t that many jobs in that field, I joined the Ambulance Service in Berkshire then later Edinburgh and really enjoyed it. Getting a taste of the medical world, I found myself delving further into the area I’d always avoided and did a shortened course for graduates in adult nursing at Napier University, Edinburgh, and so my nursing career began.
“My first job was back in Cornwall as an intensive care nurse and I really thrived in that fast paced, highly pressurised environment. I then moved into cardiology before going on to being a practice educator for radiology and cath labs, teaching staff and making sure that they were equipped with the knowledge needed to deliver high quality care safely. At this time I started learning and teaching human factors, which looks at teamwork, tasks, human performance and how error can occur in highly complex environments and systems which can trap errors and improve safety for patients.
“It was around then that my beloved dad was diagnosed with Motor Neurone Disease (MND) and given between two and five years to live.
“He was unwell for a while and initially it was suspected that he’d had a stroke or similar, so it was quite a shock when he received the diagnosis. It is the diagnosis you always dread.
“Unfortunately, he wasn’t able to receive any specialist care in Cornwall and he deteriorated very quickly with the disease, losing his ability to swallow and speak. He passed away nine months later and my family were devastated.
“Looking back on his final months it was very clear to the family that there were quite a few issues with the care he received, most stemming from the fact that expert care wasn’t available.
“We spoke to the hospital about this and I decided to offer a series of lectures over the course of a week speaking to staff about MND and how a human factors approach to his care would’ve changed many of the mistakes and errors we encountered.
“I was very determined that my lecture was impactful and that going forward, future patients would receive much better support. I did six lectures a day for a week at the hospital to all staff from consultants to house-keeping.
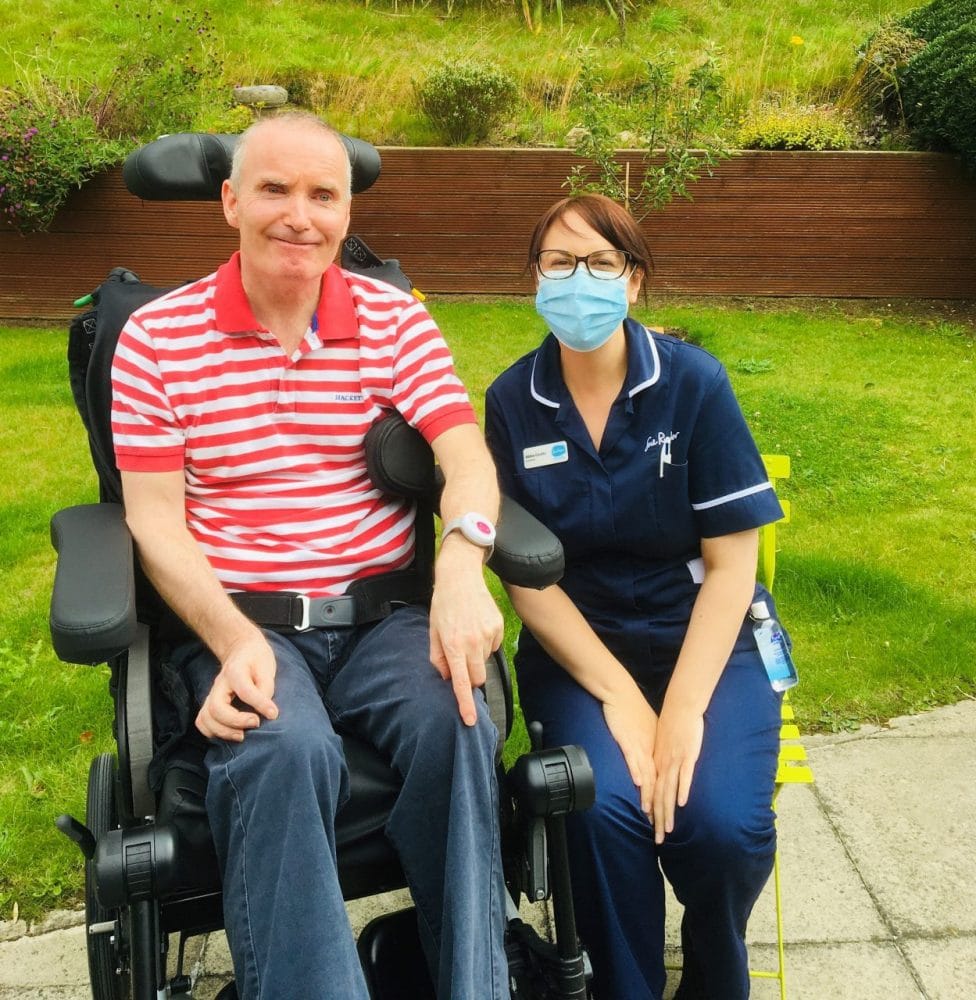
Abbie Coutts with patient Duncan May
“My dad went through a very cruel nine months in the lead up to his death and I wanted to do something to help ensure this didn’t happen again. I wanted to support the staff and raise awareness. After that I went on to give lectures about this at a palliative care conference in Aberdeen and in 2018 I spoke at the Manchester Patient Safety Conference.
“When I was offered the nursing lead role at Sue Ryder Neurological Care Centre Dee View Court in July last year, it was like I was facing the biggest nemesis possible. I had actually applied for the practice educator role but they must have seen how passionate I was about the importance of safety in care and felt I was a perfect fit for the lead nurse position.
“I had given so much of myself to the lectures I really didn’t think I’d have the capacity to nurse people in the same situation as my dad.
“At the same time, I was very drawn to the job and knew it would give me the opportunity to ensure that the residents there would receive a standard of care that my own dad should have had and deserved to receive. So I accepted the job and worked in the role until May of this year, when I moved into to the practice educator role at the centre, which had since come up again.
“In this role I have been teaching using a human factors approach since day one. This involves looking at how certain factors influence how we behave and realising that we can’t rely on humans not to make mistakes, so putting processes and systems in place to trap error before it occurs. This ensures that my high standards of safety in care are absorbed by my colleagues and in turn rolled out across the centre.
“I am also responsible for the induction of staff, monitoring their training and making sure that our staff is fully aware of the condition each of our residents is living with, the difficulties they face and the development of a clear bespoke action plan for each. The care delivered at our centre is very person centred and tailored for each individual, which in turn makes it safe.
“I think it’s true to say that my dad’s experience really does fuel my practice every day in making sure the residents at Dee View receive the best possible care and that the staff are supported in their practice.
“My overall goal is to make sure that no resident ever has to endure what he did. Not always consciously, I seem to have made it my life’s work to do what I can to ensure that history doesn’t repeat itself. I know that my dad would be proud of this career choice.”









